Billing for Mental Health Therapists in USA: How Smarter Revenue Strategies Improve Practice Growth
Mental health practices across the USA are experiencing unprecedented demand. From private therapy clinics and counseling centers to psychiatric groups and telehealth providers, more professionals are expanding their services to meet rising patient needs. Yet despite this growth, many therapists still struggle with one major operational issue: billing.
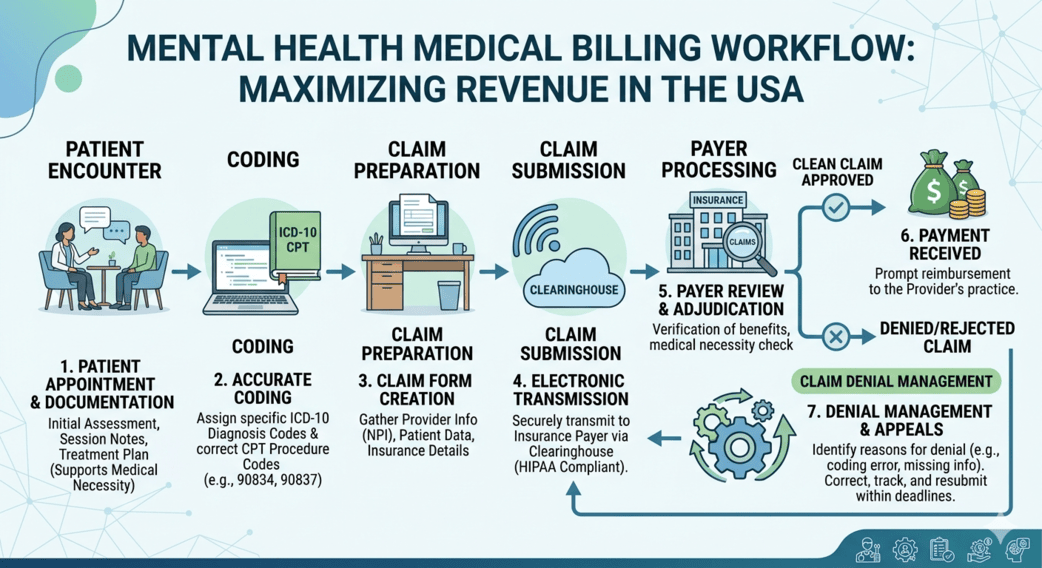
Billing for mental health therapists is far more complex than simply submitting claims. Every session, modifier, authorization, diagnosis code, and payer rule can directly affect reimbursement. A single documentation error or coding mismatch may delay payments for weeks.
That’s why many therapy practices are now investing in professional mental health insurance billing services to improve cash flow, reduce denials, and free clinicians from administrative overload.
In this guide, we’ll explore how modern mental health billing works, why outsourcing is becoming increasingly popular, and what therapists should look for in a trusted billing partner.
Why Billing Challenges Are Common in Mental Health Practices
Unlike many medical specialties, mental health billing involves unique variables that constantly change between payers.
Therapists often deal with:
- Prior authorization requirements
- Time-based CPT coding
- Telehealth billing updates
- Frequent payer policy changes
- Documentation compliance standards
- Coordination of benefits issues
- Claim denials due to coding inconsistencies
For independent therapists or small behavioral health clinics, handling these responsibilities internally can quickly become overwhelming.
Even highly experienced clinicians may lack the time needed to monitor insurance rules, submit appeals, or track aging claims effectively.
This is where a professional mental health billing specialist can make a measurable difference.
The Real Cost of Inefficient Mental Health Billing
Many therapy practices underestimate how much revenue leakage occurs from small billing mistakes.
Common financial losses include:
Missed Claims
Busy providers may forget to submit claims within payer deadlines.
Under-Coding Sessions
Incorrect CPT selection often leads to lower reimbursement than deserved.
Rejected Authorizations
Improper eligibility verification or expired approvals can result in unpaid sessions.
Delayed Payments
Even minor demographic errors may trigger claim rejections.
Increased Administrative Burnout
Therapists spending hours on billing tasks lose valuable patient care time.
Over time, these issues affect profitability, staff morale, and patient experience.
That’s why outsourced mental health billing has become a preferred solution for practices seeking long-term operational stability.
What Does a Mental Health Billing Company Actually Do?
A reliable mental health billing agency handles much more than claim submission.
Most comprehensive services include:
Insurance Verification
Checking patient eligibility before appointments reduces claim denials later.
Authorization Management
Monitoring approvals and treatment limits prevents reimbursement interruptions.
CPT and ICD-10 Coding
A skilled mental health billing and coding company ensures accurate coding based on therapy type, session length, and diagnosis documentation.
Claim Submission
Clean claims are submitted electronically to minimize rejections.
Denial Management
The billing team investigates denied claims, corrects errors, and handles appeals.
Payment Posting
Payments are reconciled properly to maintain accurate financial records.
Revenue Reporting
Detailed reports help providers track collections, aging claims, and overall performance.
A strong mental health medical billing solution creates smoother workflows while helping therapists stay focused on patient outcomes rather than paperwork.
Why Therapists Are Choosing to Outsource Billing
Outsourcing has become increasingly common among behavioral health providers throughout the USA.
Instead of maintaining a large internal billing department, many clinics now outsource mental health billing services to experienced specialists.
There are several reasons behind this shift.
Reduced Administrative Burden
Therapists already manage emotional, clinical, and compliance-related responsibilities daily. Outsourcing removes much of the operational stress tied to insurance billing.
Improved Revenue Collection
The best mental health billing agency understands payer-specific requirements and follows up aggressively on unpaid claims.
Faster Claim Processing
Dedicated billing teams typically submit claims more efficiently than overloaded front-office staff.
Lower Operational Costs
Hiring and training internal billing employees can become expensive over time.
Better Compliance
An experienced mental health billing consultant stays current with changing regulations and coding standards.
For growing practices, mental health medical billing services outsourcing often creates a more scalable business model.
Key Features of the Best Mental Health Billing Agency
Not all billing providers deliver the same quality of service. Choosing the right partner requires careful evaluation.
Here are the most important qualities to look for.
Behavioral Health Specialization
Mental health billing differs significantly from general medical billing. Work with a mental health billing provider that understands psychotherapy coding, telehealth regulations, and behavioral health payer policies.
Transparent Reporting
The best companies provide clear reporting dashboards showing collections, denials, claim status, and payment trends.
Strong Communication
Reliable support matters. Practices should receive timely updates and responsive assistance whenever billing concerns arise.
Denial Resolution Expertise
A top outsource mental health billing company actively manages denied claims instead of simply resubmitting them.
HIPAA Compliance
Security and patient confidentiality should always remain a priority.
Scalable Services
As practices grow, billing systems should adapt without disrupting operations.
Choosing the best outsource mental health billing and coding company can significantly improve financial consistency over time.
Common CPT Codes Used in Mental Health Billing
Accurate coding is essential for proper reimbursement.
Some frequently used psychotherapy CPT codes include:
| CPT Code | Description |
|---|---|
| 90791 | Psychiatric diagnostic evaluation |
| 90832 | 30-minute psychotherapy session |
| 90834 | 45-minute psychotherapy session |
| 90837 | 60-minute psychotherapy session |
| 90847 | Family psychotherapy with patient present |
| 90853 | Group psychotherapy |
Incorrect coding is one of the most common reasons claims are delayed or denied.
A professional mental health medical billing services team ensures codes align properly with session duration and clinical documentation.
Telehealth Has Changed Mental Health Billing
Virtual therapy services expanded rapidly in recent years, especially across the USA.
While telehealth creates greater patient accessibility, it also introduces new billing complexities.
Therapists must now manage:
- Telehealth-specific modifiers
- Place of service codes
- State licensing rules
- Insurance coverage variations
- Audio-only billing limitations
A knowledgeable mental health insurance billing specialist can help practices stay compliant while maximizing reimbursement opportunities for virtual care.
Signs Your Practice Needs Professional Billing Support
Many therapists wait too long before seeking outside billing assistance.
Here are some warning signs that indicate it may be time to partner with a mental health billing agency:
- Claims are frequently denied
- Payments arrive slowly
- Staff feel overwhelmed
- Revenue fluctuates unpredictably
- Therapists spend evenings handling paperwork
- Insurance follow-ups remain incomplete
- Aging AR continues growing
If these issues sound familiar, billing services for mental health therapists may provide immediate operational relief.
How Revenue Cycle Management Improves Mental Health Practices
Successful billing goes beyond submitting claims.
Modern revenue cycle management services focus on optimizing the entire financial process from patient intake through final payment collection.
For behavioral health practices, effective revenue cycle management can improve:
- Eligibility verification accuracy
- Claim acceptance rates
- Denial recovery
- Payment turnaround time
- Financial forecasting
- Operational efficiency
Strong revenue management strategies allow providers to maintain healthier cash flow while reducing administrative disruptions.
The Importance of Credentialing in Mental Health Billing
Insurance credentialing is another critical factor often overlooked by therapy practices.
Without proper payer enrollment, therapists may face claim denials even when services are medically necessary.
Professional credentialing services help providers:
- Complete payer applications
- Maintain active enrollment status
- Prevent credentialing lapses
- Expand insurance network participation
- Reduce reimbursement delays
For new therapy practices especially, credentialing support can accelerate revenue generation significantly.
How Medical Coding Impacts Behavioral Health Reimbursement
Coding accuracy directly affects whether claims are approved or rejected.
Professional medical coding services ensure:
- Proper CPT selection
- Correct ICD-10 diagnosis mapping
- Modifier accuracy
- Documentation compliance
- Reduced audit risk
Many therapy practices also benefit from integrated medical billing and coding services because billing and coding errors are often closely connected.
When both systems work together efficiently, reimbursement becomes faster and more predictable.
Real-World Example: Small Practice, Big Improvement
Consider a small counseling center with three licensed therapists handling billing internally.
The front-desk coordinator was responsible for scheduling, insurance calls, claim submissions, and payment posting. Over time, claim denials increased and aging accounts exceeded 90 days.
After partnering with a professional mental health billing services agency, the practice experienced:
- Faster insurance reimbursements
- Reduced denial rates
- Improved patient billing accuracy
- More predictable monthly revenue
- Less staff burnout
Within several months, the therapists were spending more time on patient care instead of insurance follow-ups.
This scenario is becoming increasingly common across behavioral health practices nationwide.
Choosing the Right Billing Partner for Long-Term Growth
Therapists should view billing support as a strategic investment rather than just an administrative expense.
A reliable professional mental health billing company contributes directly to:
- Financial stability
- Staff efficiency
- Reduced stress
- Better patient experiences
- Practice scalability
Before selecting a provider, practices should evaluate:
- Behavioral health experience
- Reporting transparency
- Communication quality
- Technology integration
- Denial management capabilities
- Compliance standards
Finding the right mental health billing companies can create sustainable operational improvements for years to come.
Why Many USA Practices Trust Specialized Billing Providers
Healthcare reimbursement continues evolving rapidly. Insurance regulations, coding updates, and payer requirements are becoming more complex every year.
That’s why specialized providers like 247 Medical Billing Services are helping healthcare organizations streamline operations through comprehensive support solutions.
Many therapy practices today benefit from integrated:
- Medical billing services
- Medical coding services
- Medical billing and coding services
- Revenue cycle management services
- Credentialing services
When these systems work together efficiently, providers can focus more on patient outcomes and less on administrative burdens.
Conclusion
Billing for mental health therapists is no longer a simple back-office task. It has become a critical part of practice sustainability, compliance, and long-term growth.
From insurance verification and coding accuracy to denial management and reimbursement tracking, every step in the billing process matters.
As behavioral health demand continues rising across the USA, many providers are turning toward outsourced mental health billing solutions to improve efficiency and strengthen financial performance.
Whether you operate a solo therapy practice or a growing behavioral health organization, partnering with an experienced mental health billing specialist can help reduce stress, improve collections, and support better operational outcomes over time.
FAQs
What are mental health insurance billing services?
Mental health insurance billing services handle claim submission, coding, insurance verification, denial management, and reimbursement tracking for therapy and behavioral health providers.
Why should therapists outsource mental health billing services?
Outsourcing helps reduce administrative workload, improve claim accuracy, minimize denials, and increase overall revenue collection efficiency.
What does a mental health billing specialist do?
A mental health billing specialist manages coding, insurance claims, payment posting, denial appeals, and payer communication specifically for behavioral health services.
How do mental health billing companies improve reimbursement?
Experienced billing providers submit cleaner claims, monitor payer requirements, correct coding errors quickly, and follow up aggressively on unpaid claims.
Are telehealth therapy sessions billed differently?
Yes. Telehealth billing often requires specific modifiers, place-of-service codes, and payer-specific documentation requirements.
What should therapists look for in a billing company?
Providers should look for behavioral health expertise, transparent reporting, denial management experience, HIPAA compliance, and strong communication support.
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- Jeux
- Gardening
- Health
- Domicile
- Literature
- Music
- Networking
- Autre
- Party
- Religion
- Shopping
- Sports
- Theater
- Wellness



